Ensuring good eye health in the Community
- 19
- Feb
Good eye health depends on availability of accessible and affordable eye care services for preservation and restoration of vision in the community. VISION 2020 – The Right to Sight is a global initiative launched in 1999 by the World Health Organization together with the more than 20 international non-governmental organizations involved in eye care, prevention and management of blindness that form the International Agency for the Prevention of Blindness (IAPB). It emphasizes the elimination of blindness from cataract, trachoma, onchocerciasis, refractive error, vitamin A deficiency, and other causes of blindness in children by the year 2020. The goal of Vision 2020 is to enable all persons to receive eye care and have the right to sight – which is one of their fundamental human rights (Foster, 2008). The core areas of strategy are human resource development, infrastructure and technology development, disease control, advocacy, and partnerships and collaboration among stakeholders in eye health (Foster, 2008). Ten years after commencement, the impact of the initiative has been felt worldwide in a 10 to 13 percent reduction in visual impairment (Ackland, 2012).

Universal Eye Health
To further improve eye health, in 2013, the World Health Assembly endorsed a resolution tagged “Universal eye health: a global action plan 2014–2019 – ensuring that all people have access to needed promotive, preventive, curative and rehabilitative health services, of sufficient quality to be effective, while also ensuring that people do not suffer financial hardship when paying for these services”.
Human resources for eye health
Ophthalmologists and Allied eye care workers are needed to improve eye care services in the community. In Nigeria, Specialist training is provided by accredited training institutions and evaluation conducted by the National Postgraduate Medical College of Nigeria and the West African Postgraduate Medical College.
In 2014, I was elected to the coveted post of the Chairman and Chief Examiner of the Faculty Board of Ophthalmology of the National Postgraduate Medical College of Nigeria. The Faculty oversees the training of Ophthalmologists competent to lead the eye care team for effective eye care delivery. Since 1984, the number of graduating Ophthalmologists has gradually increased to a total of 343.
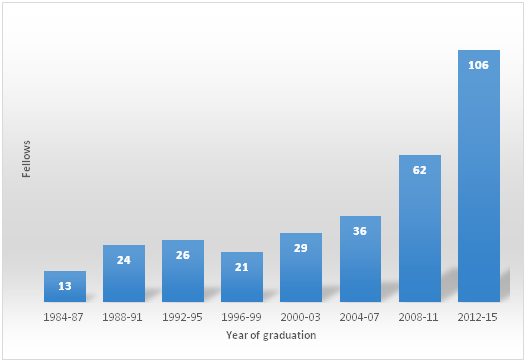
This means that for Nigerians, with a population of 182 Million, the College has been able to produce 1 Ophthalmologist to 530,000 Nigerians, as against the WHO target of 1 Ophthalmologist to 250,000 people (IAPB, 2014). We do not have enough Ophthalmologists to manage eye diseases in Nigeria. Achieving the goals of the new WHO Action plan (a 25% reduction in blindness and visual impairment by 2019) for Universal eye health coverage will be impossible without addressing the eye health workforce crisis (WHO, 2013).
By the grace of God, I have contributed to the training of not less than 24 Ophthalmologists while 19 other doctors are currently in training.
Why would you keep your trade to yourself and not pass it on to the next generation?
Incorporating Eye Health Care within the Primary Health Care
The Alma-Ata Declaration of 1978 expressed the need for urgent action by all governments, health and development workers, and the world community to protect and promote the health of all people. In achieving the goals of Universal Eye Health, it is desirable to incorporate Primary Eye Care (PEC) within the pre-existing Primary Health Care to effectively reach rural communities. In furtherance of this, we conducted a study to assess the human and material resources available for primary eye-care delivery in rural communities. We found that in 27 health facilities available in Atakunmosa LGA, forty-one (42%) community health extension workers, 42 (43%) health assistants, 3 (3%) community officers of health and 11 (11%) registered nurses administered PHC. No worker had training in PEC and none of the centres had all the materials for basic PEC delivery. Although procurement of materials and training of health-workers in basic PEC delivery is required, the healthcare facilities and workers currently available were found to be adequate to commence integration of PEC into the PHC system. (Onakpoya, Adeoye et al, 2009).
It is heartwarming to note that only last month, the Federal Ministry of Health launched the Rapid Result Initiative programme, called: “Better Health for all,” made to produce quick and visible impact on the lives of every Nigerian especially, the most vulnerable and poor in the society. Under this programme, 110 Primary Health Centres all over Nigeria would be revamped within 100 days. It is hoped that by this, health care delivery will be brought closer to the underserved communities.
